Image

Bay Area Hospital in Coos Bay.
|
COURTESY OF BAY AREA HOSPITAL
Image

PROVIDENCE, A HEALTH SYSTEM WITH HOSPITALS AND CLINICS ACROSS THE WEST, INCLUDING PROVIDENCE ST. PATRICK HOSPITAL IN MISSOULA, MONTANA, REPORTED A NET OPERATING LOSS OF $510 MILLION FOR THE FIRST THREE MONTHS OF 2022./KATHERYN HOUGHTON/KHN
Image

The Knight Cancer Research Building at Oregon Health & Science University.
|
COURTESY OHSU
Image
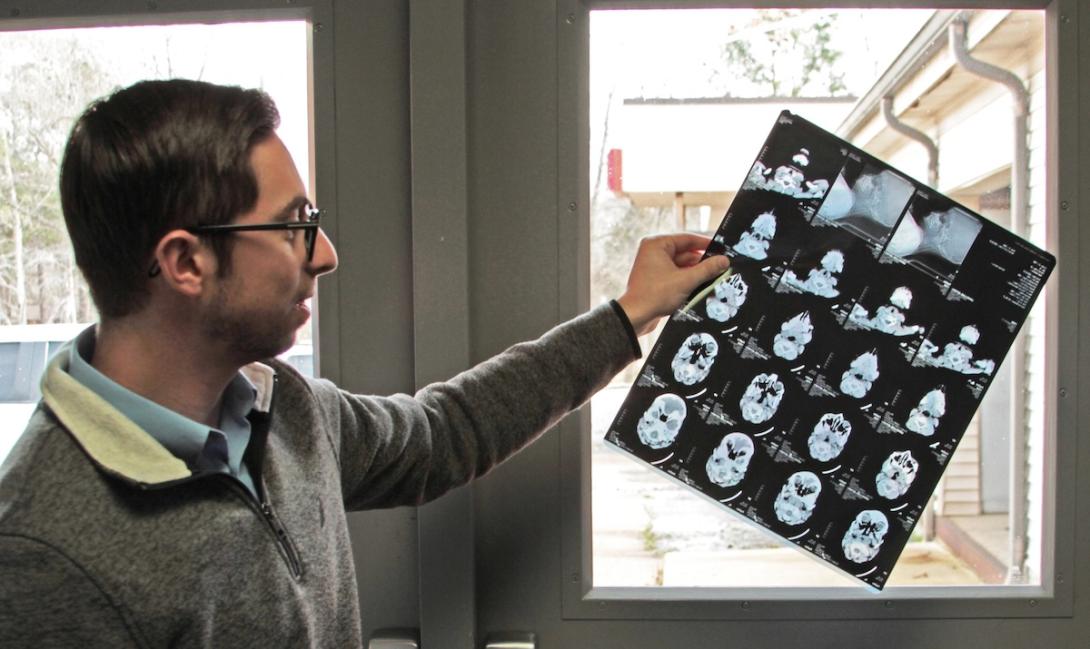
KYLE KOPEC, BRADEN HEALTH’S CHIEF COMPLIANCE OFFICER, HOLDS UP A SAMPLE OF DIAGNOSTIC IMAGES LEFT BEHIND AT A TENNESSEE HOSPITAL. AS THE COMPANY TAKES OVER ABANDONED HOSPITALS, A MAJOR TASK IS FIGURING OUT WHAT TO DO WITH OLD MEDICAL RECORDS STACKED IN BOXES./BLAKE FARMER/KAISER HEALTH NEWS
Image

Gov. Kate Brown.
|
SHUTTERSTOCK
Image

Gov. Kate Brown.
|
SHUTTERSTOCK
Image

THE BULLETIN
Image

THE $50-MILLION SKY LAKES COLLABORATIVE HEALTH CENTER IN KLAMATH FALLS IS A COLLABORATION BETWEEN OHSU AND SKY LAKES MEDICAL CENTER./SKY LAKES MEDICAL CENTER