Image

The Bull of Wall Street in Manhattan in New York City.
|
ALEXANDER NAUMANN/PIXABAY
Image
TOWFIQU BARBHUIYA/UNSPLASH
Image
SHUTTERSTOCK
Image
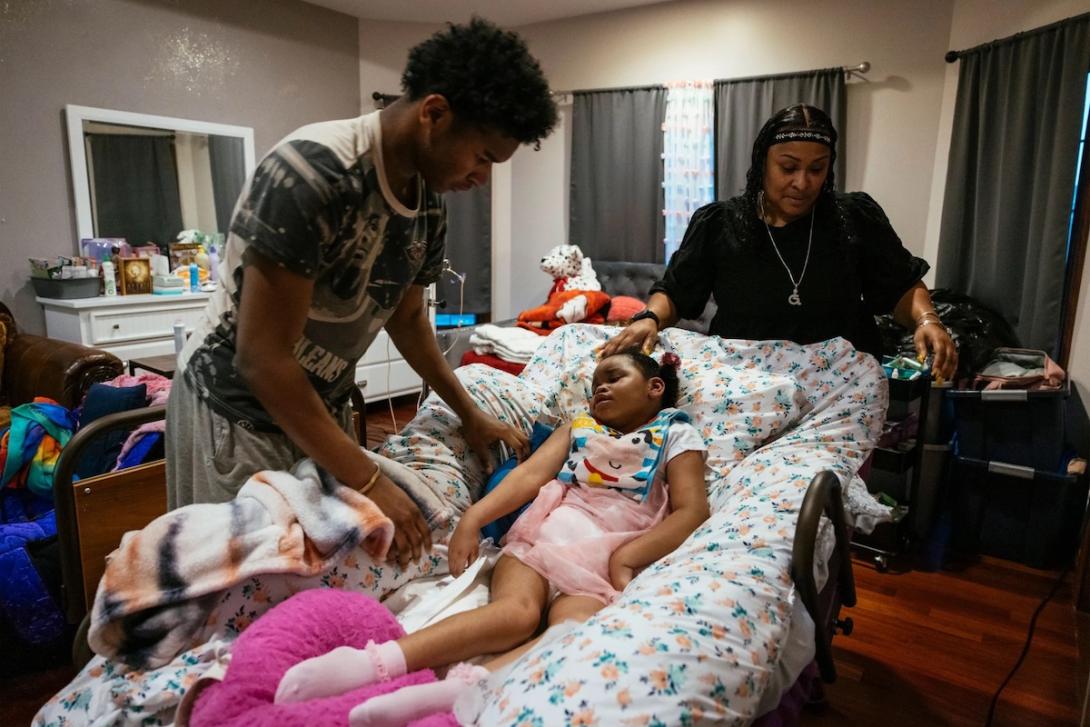
RHONDA JONES WITH SON TYRUS AND DAUGHTER ALAYNA AT THEIR HOME IN CROWN POINT, INDIANA. ALAYNA WAS INJURED DURING HER BIRTH AND HAS CEREBRAL PALSY. SHE WAS RECENTLY HOSPITALIZED WITH RESPIRATORY SYNCYTIAL VIRUS, OR RSV./TAYLOR GLASCOCK/KHN
Image

SHUTTERSTOCK
Image
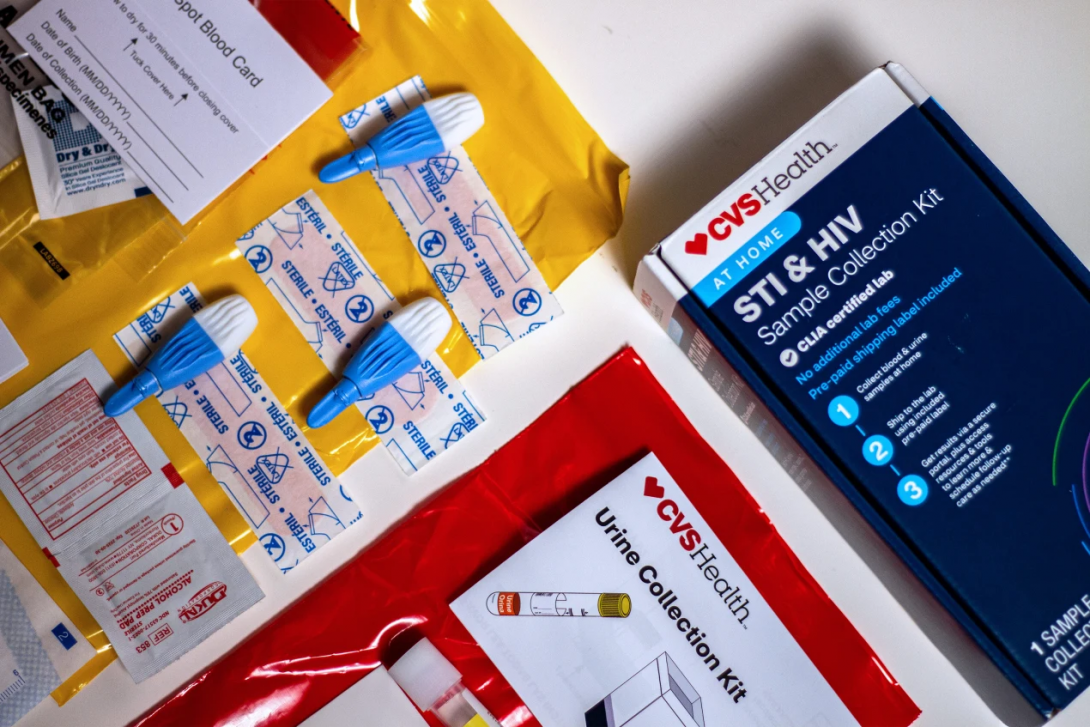
CVS’ AT-HOME TESTS THAT SCREEN FOR HIV AND OTHER SEXUALLY TRANSMITTED INFECTIONS CAN BE BOUGHT IN STORES AND ONLINE. THE KIT IS PRICED AT $99.99./ERIC HARKLEROAD/ KHN
Image

JACQUELINE LEWIS LOST SON SHAUN LEWIS TO AN OVERDOSE IN OCTOBER 2022. SHE’S NOW RAISING HER 7-YEAR-OLD GRANDDAUGHTER, WHILE CARING FOR HER 95-YEAR-OLD MOTHER WHO HAS DEMENTIA, ON NOTHING MORE THAN SOCIAL SECURITY PAYMENTS./MADDIE MCGARVEY/KHN
Image

TWO-YEAR-OLD ZION GASTELUM DIED FOUR DAYS AFTER RECEIVING BABY ROOT CANALS AND CROWNS AT KOOL SMILES, A PRIVATE EQUITY-AFFILIATED DENTAL CLINIC IN YUMA, ARIZONA./SCREENGRAB OF ABC15 ARIZONA BROADCAST
Image
SHUTTERSTOCK
Image

MOHAMED HASSAN/PIXABAY