Image

SHUTTERSTOCK
Image

DANIEL AGRELO/PIXABAY
Image

SABINE VAN ERP/PIXABAY
Image

GUNDULA VOGEL/PIXABAY
Image

GUNDULA VOGEL/PIXABAY
Image

WHEN MARVIN QUERRY, WHOSE WIFE, DIANE, LIVES AT THE BARONE ALZHEIMER’S CARE CENTER IN NEVADA, MISSOURI, HEARD THE CENTER MIGHT CLOSE, HE STARTED AN ONLINE PETITION PROTEST AND SPENT NEARLY $3,000 TO RUN ADS (PICTURED) IN THE LOCAL NEWSPAPER./KHN PHOTO ILLUSTRATION/MARVIN QUERRY
Image
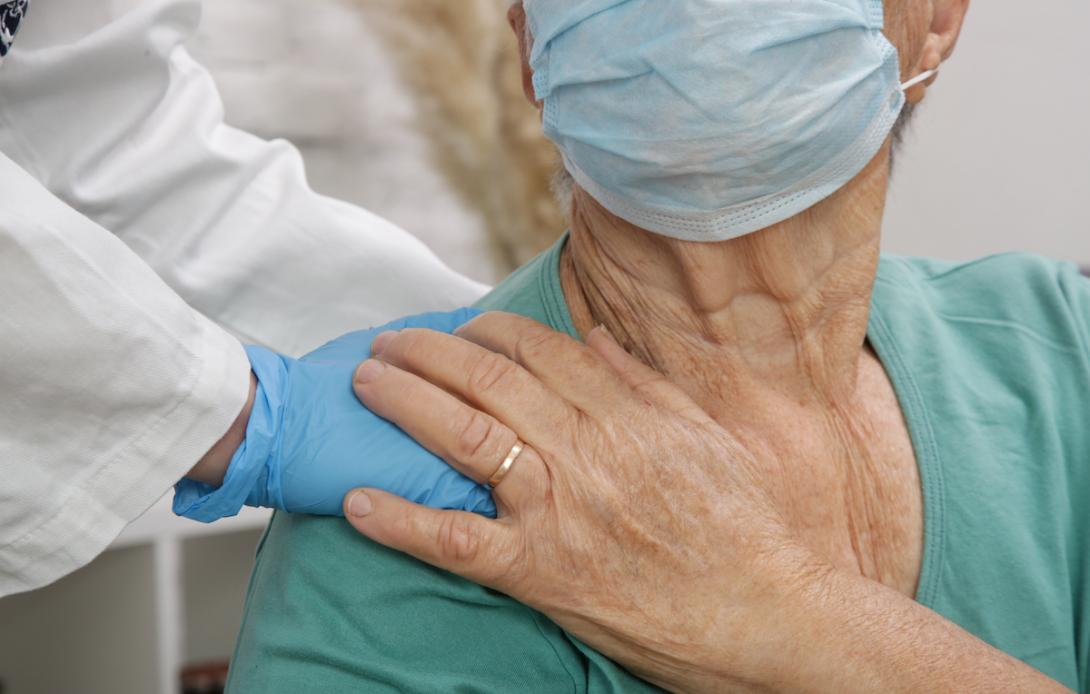
SHUTTERSTOCK
Image

Nursing home visit Raul Lugo wanted to hug his grandmother Rosa Perez, 89, during their in-person visit at her nursing home./Courtesy of Damary Lugo
Image

NURSING HOMES HAVE HAD TO COBBLE TOGETHER PROTECTIVE GEAR./COURTESY OF PAMELA BLACK/KAISER HEALTH NEWS.
Image

Southeast Portland nursing home Healthcare at Foster Creek.
|
DAVE KILLEN/THE OREGONIAN