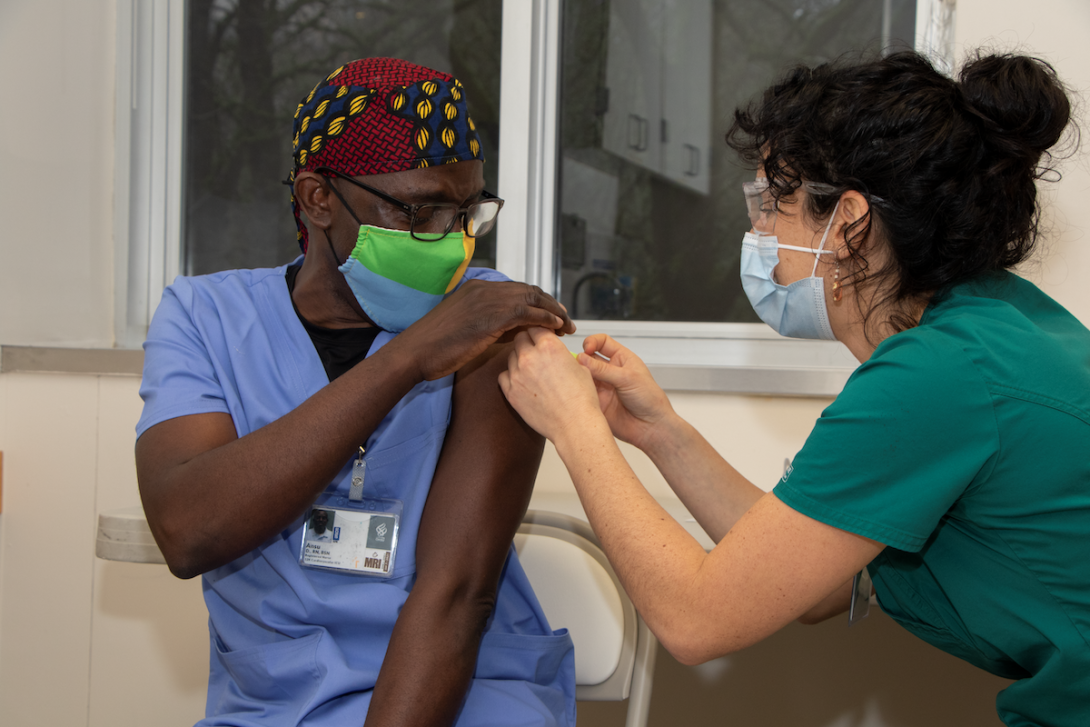
With the COVID-19 pandemic, punctuated by protests for racial justice, there is heightened recognition of racial inequities in this country. This pandemic has been an important opportunity thus to see more clearly, and to follow words with action. While there has been some progress to address these inequities, there have been many challenges.
Two months into the vaccine rollout here in Oregon, we see a troubling trend. Already disproportionately affected by the virus, Black and Brown communities have thus far been receiving vaccines at much lower rates than their white counterparts. At the time of this writing, 10% of white Oregonians have received a vaccine compared to 8.2% of Black Oregonians and 4.2% of Latino Oregonians. Nationwide surveys show only 26% of Black Americans and 37% of Latino Americans say they would get a COVID-19 vaccine if available. A full 43% of Latino Americans however say they are waiting to see others vaccinated first before considering taking a vaccine themselves. Black and Brown communities are not a monolithic group with a singular ‘misunderstanding’ of the benefits or risks of the vaccines, but people on a spectrum of hesitancy, with varying concerns that range from the implausible to possible to almost certain. In the excitement and hope of the vaccination rollout, what we do and how we do it has never been more important. “Community immunity” requires the vast majority of the population to be vaccinated to get to the other side of this pandemic; we must do so with equity at the forefront of our collective efforts.
The communities that keep society functioning are the essential workers who bear the brunt of this pandemic: a diverse group trying to make the best decisions for themselves and their families in the face of ever-mounting pressures from an unrelenting and mutating virus. Most have experienced firsthand how systems continue to fail them, before and during this pandemic. They see that getting a vaccine is no more a panacea than a minimum wage has guaranteed them the American dream, or SNAP benefits have saved them nights without hunger, or housing assistance has ensured them access to a good school and a healthy neighborhood, or health insurance has guaranteed them access to care. Overrepresented by people of color, their unwillingness to get a vaccine is in part rooted in prior experiences. It is our responsibility as participants in the healthcare system to listen and prove ourselves worthy of the trust of those who have the least reason to do so.
What Community Members Can DoIf you are vaccinated or planning to be, share why and how to help dispel myths.
Share information and stories with family, friends, and on social media. Especially if you are a person of color and/or speak languages other than English.
If you are in health care taking care of COVID-19 patients, share your experience.
If you have had COVID-19, or someone close to you has, share your story.
Wear a mask (or two), keep your distance, ventilate indoor spaces or go outside to socialize, wash your hands.
If you can help with logistics such as helping an older relative navigate online registration, transportation for a friend or family member, volunteer as a vaccinator etc, please offer.
If you worked on elections/community organizing, use the same strategies/tools, and offer your skills for the vaccination effort--it will require many of the same approaches and networks to get that reach.
There is now an entire discipline of research documenting many ways our medical system perpetuates racism. Studies repeatedly show the subtle and not so subtle discrimination faced by patients of color causes many to receive inferior medical care. A recent poignant example is the treatment Dr. Susan Moore received at a community hospital in Indiana. Moore recorded herself on video prior to her early death from complications of COVID-19, describing how her white doctors dismissed and ignored her requests for care, before and during her hospitalization. Recording her story in a video viewed by millions, she showed herself still hospitalized and actively short of breath, while her doctors dismissed her and aggressively sought to discharge her. Moore died ten days after hospital discharge.
Compounding these biases leading to patterns of individual negative consequences, Black Americans have lower access to comprehensive health insurance, and 67% of Black neighborhoods have a shortage of primary care access relative to white neighborhoods, a key source of access to health care. This disparity is a symptom of systemic racism, including redlining, educational segregation and discriminatory policing. Latino and Native American communities, as well as many immigrant communities of color, also face discrimination interfacing with institutions. Experiences of marginalization informs much of the hesitancy with which people of color may approach health care. That includes the COVID-19 response and now the vaccine rollout, which have unfortunately not provided a counterpoint thus far; health care and social systems have yet to equitably support our most vulnerable communities.
What Policymakers Need To DoShare your experience of vaccination as a healthcare provider, widely and specifically to your racial and cultural community.
Know your community and listen to them. Partner and support community based organizations and religious leaders who may be trusted links to interface with patients and community members marginalized by the health system.
Make culturally and linguistically specific information available to all:
WHO: who.int/emergencies/diseases/novel-coronavirus-2019/covid-19-vaccines
CDC: cdc.gov/coronavirus/2019-ncov/vaccines/index.html
Leverage the reach of the internet. Help get the word out about the high safety and efficacy of the vaccines in personalized, shareable, digestible ways, using reliable sources of information and with the talent of the dancers, singers in our communities through TikTok and other social media.
Continue to work to make vaccination efforts physically and emotionally accessible to those hardest hit by this pandemic.
The urgent need is investment in trust-building in new ways. Let us not miss the opportunity to learn from early mistakes and support those hardest hit by the pandemic. Hesitancy and low uptake can mean the difference between life and death for those most at risk. But building trust requires customization. Messaging, outreach and access for Latino communities will need to be different for a metro area Black community or a rural Native American community. All have suffered discrimination, as well as a disproportionate impact from the pandemic, but their needs are not the same. The inadequate effort towards culturally specific trust-building on the part of health care institutions means that some people may hesitate to engage with the system. Mexican immigrants, for example, who make up a large proportion of the Latino population in the Pacific Northwest, are typically pro-vaccination; their kids tend to have some of the highest vaccination rates relative to other groups. Yet, they have not been clamoring for vaccines en masse. A Kaiser Family Foundation poll recently showed that 66% of Black adults say the government’s response to the COVID-19 pandemic would be stronger if white people were getting sick and dying at higher rates than people of color. There is much work to be done.
Black and Brown people don’t want any more COVID-19 in their families, and want to go back to work or continue to work safely. Many community members and leaders have also stated clearly they want access to health care, including vaccines, with attention to relationship-based, honest information sharing, and in their preferred language. We know the gap is in trustworthiness of health systems and government agencies. Communities need outreach and support with language and cultural translation, via trusted messengers and navigators. We must relay accurate information about the vaccine, and do so in digestible, customized ways. Our communities have said what they need, and it is now time to listen and act, if we truly intend to make an impact on what really matters.
Dr. Tanya Kapka is a family medicine physician; Adelina Mart is an epidemiologist; Dr. Shimi Sharief is a nephrologist and Dr. Bukhosi Dube is an internist.