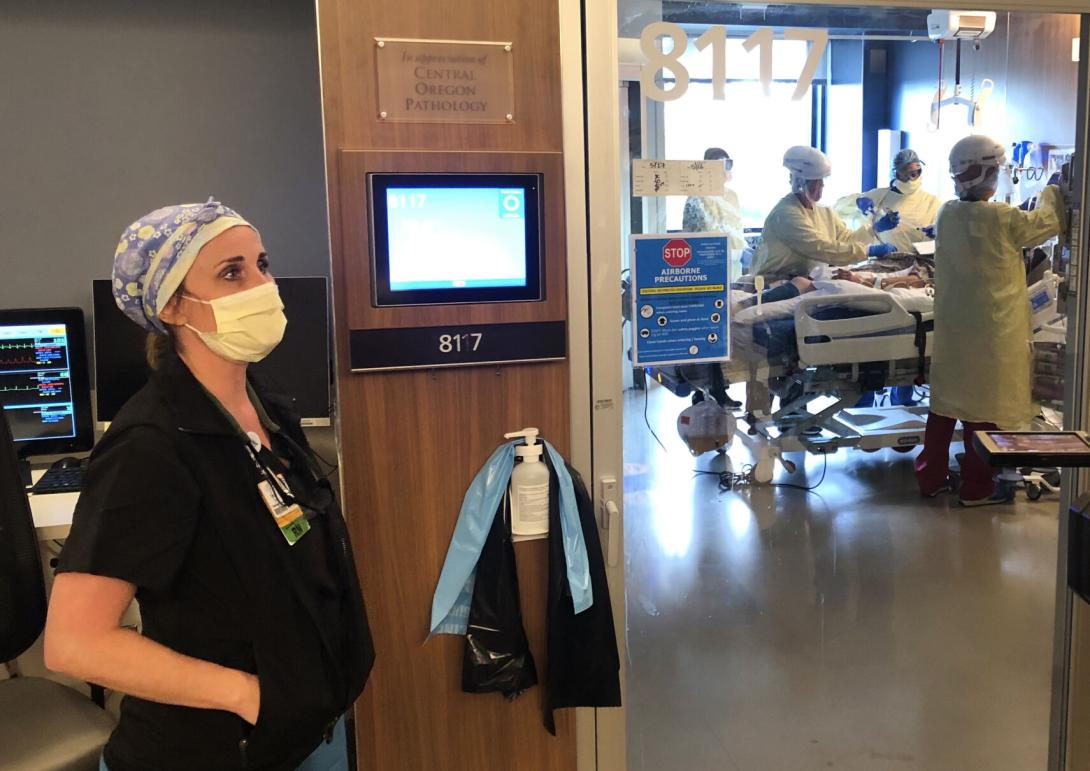
Every day that Tiffany Simmons goes to work at St. Charles Bend, she finds herself awash with despair. And every day that Jake Newton starts his shift at the same hospital, he feels like he’s in a war zone. Both are registered nurses who say the emotional weight of the pandemic, now in its 19th month in Central Oregon, has not grown any easier to shoulder.
Like other nurses at the region’s main hospital for COVID-19 patients, Simmons and Newton have been told by families that they’re not giving their loved ones proper treatment. They’ve been yelled at by patients. They’ve been told — by both patients and families — that the pandemic is a hoax. They’ve been told that they’re killing a loved one.
“I will treat every patient who walks into our doors my best and treat them with compassion and caring,” said Newton, who spoke as a member of the Oregon Nurses Association. “We’re dealing with people coming in with COVID and treating them, but they’re yelling at us that it’s a hoax or a lie and we’re not giving them the proper treatment.
“That’s why we’re burned out. That’s why people are leaving the profession. It’s our reality right now.”
Some might say the nurses are angry. Others might say they’re suffering from compassion fatigue. But they are working difficult shifts. At a time when there is a severe nursing shortage nationwide, those nurses that are working are losing coworkers because of mandates that health care professionals must be vaccinated or face being placed on leave or being fired.
It’s a tough time to be a nurse in Oregon.
Simmons, a single mother, feels like she is fighting an unseen enemy. Nineteen months into the pandemic, she’s still stripping off her scrubs in the garage and tossing them into the wash before coming into her home.
“Honestly, some days, I deal with it better than others,” said Simmons, who also spoke as a nurses association member. “Sometimes, we can be emotional, too, because we’re tired and have to rehash information over and over again. Often, it’s the psychological aspects of the work that is the most difficult.”
The battle to help sick COVID-19 patients get better is compounded by a staff shortage and the presence of a traveling workforce employed at the hospital — a workforce earning much more money than Simmons is receiving — and it leaves her discouraged.
“There are people I work with now who are leaving St. Charles to work as a traveling nurse,” Simmons said. “There’s a component of moral injury that comes from being short staffed, which was happening before the pandemic and never addressed.”
Some days, she has to eat on the run and doesn’t get a break because there’s not enough nurses to care for patients in her absence. Every morning she packs a lunch and drinks 16 ounces of water before she leaves home to prepare for a day of caring for others.
She does spend a lot of her time at work fielding calls from family members of COVID-19 patients. The hospital hasn’t allowed them to visit sick relatives since the pandemic started.
Last Monday was the governor’s deadline for health care professionals to either be vaccinated or stop working. Some could continue to work unvaccinated if the employer granted a medical or religious exemption. Simmons and Newton said that the Oct. 18 mandate has made the nursing shortage situation worse.
The nurses association illustrated the situation recently by citing a survey of nurses at the Oregon Health & Science University, where 92% said they were exhausted. More than half said they were considering leaving the profession entirely. The association represents 15,000 Oregon nurses.
Some hospitals, St. Charles included, have break nurses who float through a ward so that a nurse can take a lunch break without leaving patients in the care of another nurse who already has a full patient load. But break nurses are not a norm at all hospitals or on all floors, said Natasha Schwartz, Oregon Nurses Association board member at a recent online press conference.
The nursing association has been asking that hospitals make these break buddies mandatory at all hospitals. The association also asked the governor and the Oregon Health Authority to form a commission to assess hospital staffing models and to come up with recommendations that prevent nurse burn out.
“The current nursing crisis has been decades in the making,” Schwartz said. “We see nurses leaving the profession because of the decision not to vaccinate. We won’t be able to educate enough nurses to replace them.
“The job is difficult. We’re asking for bold action.”
The biggest issue facing the nursing profession is there’s no statewide standards, including requiring break nurses to ensure that staff get break time during a shift, said Kevin Mealy, Oregon Nurses Association communications manager.
“It’s something we push for and advocate for, but it’s in very few contracts,” Mealy said. “During a 12-hour shift, nurses are dealing with immense mental and physical challenges. People need a break to take a moment for themselves and that’s never been more important than during COVID and takes the emotional weight off nurses.”
On the hospital floor where Newton works at St. Charles Bend, he cares for about four patients at a time. These patients require a high level of care. When he’s treating COVID-19 patients they’re not allowed visitors. They can see loved ones only through an Ipad. They often feel isolated, he said.
Caring for four patients may not sound like a lot, but when constant monitoring is required there are times that Newton cannot walk away.
He’s monitoring the oxygen level of his patients, administering medication, helping patients to remain on their stomachs to allow for their lungs to be spread out as much as possible.
Caring for COVID-19 patients requires a lot of monitoring because the oxygen levels can plummet in a flash.
“The numbers of COVID-19 patients are going down slowly from the peak we had before, “ Newton said. “We’re not entirely a COVID-19 floor now, but we’re also dealing with capacity and staffing issues. We’re pretty full despite staffing issues.”
Ever since the delta variant appeared in September, Newton has felt like the virus is everywhere. Rarely does he go out on his days off because he doesn’t want to expose himself to the virus. He’s especially alarmed when he’s out at a grocery store and sees people without a mask.
“No one expected this surge. I feel like this is a country where we look out for each other, and I just don’t see that anymore,” Newton said. “COVID is obviously killing people and while the survival rate is high, many people have permanent lung damage.”
As a nurse, Newton said part of the job is to educate the patient and the family on treatment. Sometimes they don’t want to hear what he has to say.
“It’s super challenging,” Newton said. “We keep trying and keep pushing forward. That’s what we’re trained to do. Regardless of how tough it is, we are still here doing that.”