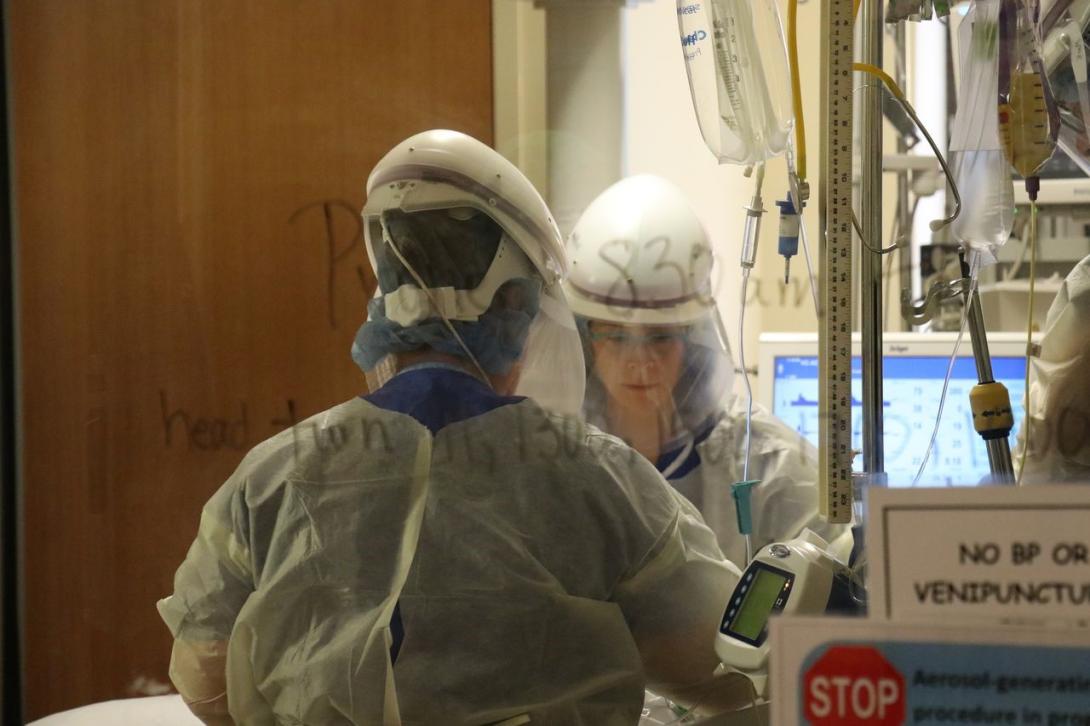
Swamped by the rapid surge in patients sick with COVID-19, Oregon hospitals are close to running out of beds.
On Wednesday, the number of people in Oregon hospitals with COVID-19 hit 850, up from 112 pandemic-related hospitalizations just five weeks ago.
To try to ease the crisis, officials are struggling for ways to create more hospital capacity to handle both COVID-19 patients and others who need care. But how much these efforts will help remains unclear.
Oregon hospitals on Wednesday had just 41 adult intensive care beds available statewide. That’s 6% of the state’s total supply of 652 intensive care beds. Availability varies from hospital to hospital and region to region. Some hospitals, especially in southern Oregon, are entirely out of intensive care beds.
But urban areas with a high demand for beds are also hard hit. In a six-county northern region of Oregon, which includes the tri-county Portland area, there are 17 intensive care beds available out of 335, or 5%.
Oregon hospitals have 292 regular adult hospital beds outside intensive care units available, about 7% of the state’s 4,193 beds.
Here’s the crucial catch: Hospitals can boost bed tallies with more staffing and equipment like ventilators. Oregon state and federal officials are in a dash to prop up the faltering system before it reaches gridlock.
It’s a complex, multifaceted plan that includes bringing in support personnel through the Oregon National Guard as well as out-of-state medical professionals, and sending some hospital patients to long-term care facilities to free up hospital beds.
If Oregon pulls it off, hospitals would move patients into long-term care facilities when they are no longer acute but still can’t return home.
This would boost hospital capacity and create a quicker pipeline to move patients through the hospital system and into other types of care. Oregon may even get a field hospital to treat more people.
Most of the plans are still a work in progress. State officials say they want to use beds in long-term care facilities, but haven’t detailed how many beds they want, how many beds are available, and where they are.
It’s also unclear where a field hospital would go. State officials submitted a request to the Federal Emergency Management Agency earlier this month and are still in talks with that agency.
It’s too soon to know if the efforts will be enough. Hospital officials are still waiting for firm details from state and federal officials about how many personnel and resources they will receive.
Meanwhile, the COVID-19 pandemic continues, driven by the delta variant. The Oregon Health Authority reported 2,139 new and presumed cases on Wednesday and a rolling seven-day average of nearly 2,000 new cases a day. Oregon logged 11 more COVID-19-related deaths on Wednesday, reaching a total toll of 2,975.
The picture is grim. Oregon Health Authority Director Patrick Allen on Thursday said more than 200 patients in emergency departments are waiting for a bed.
"Patients are parking in hallways," Allen said. "Staffing is critically short."
If the situation continues to worsen, doctors and nurses "may have to face the heart-wrenching triage decisions" about what patients they can save and cannot save due to limited resources, he said.
"We are really overwhelmed and this is really a dire situation," said Dr. Jeff Absalan, chief physician executive for St. Charles Hospital in Bend.
The bed shortage impacts patients with other serious needs too, such as heart surgeries or cancer.
In Bend, the hospital had 62 patients with COVID-19 on Thursday morning, close to 30% of the hospital's acute care beds, Absalan said.
"There are patients that have cancer, heart disease and neurological disease," he said. "they're being delayed right now. We're rationing care. Only patients that have the most severe needs for surgical care are getting that care and many, many more are waiting."
The number of COVID patients in hospitals is projected to grow. A forecast by Oregon Health & Science University estimates that 1,000 Oregonians will be hospitalized with COVID-19 on Labor Day.
Here’s a look at the state’s efforts:
Oregon Guard Mobilized
The state plans to eventually mobilize up to 1,500 Oregon National Guard troops, with a possible field hospital to take pressure off hospitals and bring in teams of nurses and other out-of-state health care professionals. The Guard members will clean hospital rooms, check temperatures of visitors and assist in other non-clinical roles at hospitals to free up medical staff to focus on patients.
The first wave of that mobilization starts perhaps by Friday, when 500 Guard members go to hospitals in Bend, Redmond, Prineville, Madras, Roseburg, Medford, Ashland, and Grants Pass, said Stephen Bomar, spokesman for the Oregon Military Department. Those hospitals are part of the St. Charles, Mercy, Asante and Providence networks.
Eventually, 1,000 more Guard members will deploy to hospitals in the Portland and Salem areas, an official said. The Guard was unable to give the time frame for that deployment.
State Officials and Feds Continue to Plan
Meanwhile, the Oregon Department of Human Services and Oregon Health Authority are moving forward with funding nurse crisis teams to aid long-term care facilities that will receive more patients.
“Teams of nurses that can be moved between long-term care facilities may be several weeks out,” Jonathan Modie, a spokesman for the authority, said in an email to The Lund Report.
The goal is for each team to have a registered nurse or licensed practical nurse and four certified nursing assistants, though that’s still in the planning stage, Modie said.
Allen said Thursday there will be eight nurse crisis teams. Four of them will start in September in southern and central Oregon hospitals. Four more will arrive in October.
Separately, the state is concentrating on bringing in contract clinicians into six hospitals in central and southern Oregon with immediate acute care needs, Modie said.
It’s too soon to estimate how many will go to each hospital from the national travel clinician market, Modie said, adding that the state will have a better sense within a week.
Oregon has requested help from other states through an emergency management assistance compact. It seeks 35 physicians, 35 advanced practice providers, 300 registered nurses, 10 paramedics, and 100 respiratory technicians for temporary assignments in central and southern Oregon, the health authority said in a bulletin to providers.
“Our hospitals in every hospital region in Oregon are at or over capacity. Addressing these needs is an urgent state goal,” the authority said in the bulletin to Oregon health care providers and public officials this week.
The state’s also tapping its Oregon network of volunteer health care workers and encouraging providers to register with SERV-OR, the state’s registry of volunteers.
The first group of volunteers -- seven nurses -- arrived Monday at St. Charles Health System in central Oregon, Modie said.
The health authority is also cutting red tape with state licensing agencies to make it easier for health care providers with out-of-state licenses to work in Oregon. For example, the Oregon State Board of Nursing adopted rules that let licensed nurses and certified nursing assistants outside Oregon have emergency authorization during this crisis. Similar steps are in place for out-of-state physicians and physician assistants in good standing in their states.
State officials are encouraging hospitals and health care providers to guide their patients to take steps to keep usage down where possible.Those steps include encouraging patients to get a COVID-19 vaccination and advising them to go to urgent care clinics for health issues that don’t need an emergency room.
Hospitals Wait For Relief
At Providence Medford Medical Center, officials expect 75 Guard members to arrive on Thursday.
They will take temperatures at entrances, check badges, deliver and stock supplies and assist with dietary work, wash dishes, clean rooms and unload freight, said Liz Del Valle, a spokeswoman for the hospital.
“The additional staff will allow our medical staff to focus entirely on providing medical care to patients, without distraction and interruption,” she said. “Today our nurses are helping to clean rooms and other duties that aren’t the best use of their expertise. The intent is to make sure our employees are able to work at the top of their license and skill level.”
Del Valle said the hospital hopes to take non-clinical caregivers who are experienced with patients and transition them into roles to support patient care.
“We will work with Guard members to make sure they have some consistency with what they are doing so once they are trained, they continue to do that same work while they are here,” Del Valle said, adding that their deployment is initially for six weeks.
The Medford hospital still needs nurses and other clinical staff and efforts to secure those are underway, Del Valle said.
The hospital has about 30 COVID-19 patients. That’s twice its level of COVID-19 patients during the January peak, which was closer to 15, Del Valle said. On July 1, the hospital didn’t have any patients with COVID-19.
The 136-bed hospital and its 15 intensive care beds are full. No beds are available and the hospital is doubling up patients in some areas, including its intensive care unit to make room.
Elective surgeries are canceled and average wait times in the emergency room are 90 minutes.
The biggest problems are a lack of staffing and beds, Del Valle said.
Asante, which owns Ashland Community Hospital, Rogue Regional Medical Center and Three Rivers Medical Center, expects 150 Guard personnel.
As with Providence, they’ll work in support roles and “will free up our employees to resume regular duties,” said Asante spokeswoman Lauren Van Sickle.
The three hospitals had 149 COVID-19 patients on Tuesday evening, with no intensive care beds available.
The health system has canceled all elective procedures and surgeries, including screenings such as colonoscopies.
The biggest challenge is the number of post-acute care patients who are waiting to get into a long-term care facility or nursing home and its impact on the availability of hospital beds, Van Sickle said.
“If those beds were made available, that would allow us to move patients from the emergency department into one of the units more quickly, and possibly resume some elective surgeries and procedures,” she said in an email.
Asante continues to ask the state for more resources, including ventilators and oxygen and wants the state’s help in coordinating discharges for patients after they exit acute care, including possibly transferring patients to facilities out of the area.
A spokeswoman for Providence Portland Medical Center would not answer questions from The Lund Report about the hospital’s bed supply, COVID-19 patient volume and what resources it needs.
At Mercy Medical Center in Roseburg, a nonprofit faith-based hospital, officials need more clinical staff, including respiratory therapists and acute care registered nurses, spokeswoman Sarah Baumgartner said.
The hospital has added four intensive care unit beds and has 20 now.
Overall, the hospital is running at 93% to 100% capacity as measured in bed usage, which shifts as admissions and discharges happen, Baumgartner said.
Its COVID-19 patient count varies, but has exceeded more than 50 patients on one day at the 121-bed hospital. In comparison, the hospital had about 10 COVID-19 patients three weeks ago.
Like most other hospitals, Mercy Medical Center has canceled elective procedures. But that’s not been enough to dampen the inflow of patients.The biggest problems are “too many patients and too few staff,” which is due to illnesses, pre-existing staff shortages and the delay in getting patients out to skilled nursing facilities, Baumgartner said.
For now, the hospital is asking state officials to “be mindful of rolling out well-meaning mandates during a crisis,” she said. That’s because more mandates could put an added strain on staffing levels and cripple care teams, she said.
St. Charles Health System, which operates hospitals in Bend, Redmond, Madras and Prineville, said it will get 150 Guard members on Thursday. They’ll be there through the end of September.
“We are tremendously grateful for the Oregon National Guard members who are leaving their jobs and families to answer our hospitals’ call for help,” said Joe Sluka, St. Charles’ president and CEO, in a statement. “While they will not be providing bedside care to patients, they are going to be bridging gaps in staffing elsewhere in the system that are critical to our operations.”
You can reach Ben Botkin at [email protected] or via Twitter @BenBotkin1.
I havent seen coverage of this depth anywhere else. Thank you!